Employee healthcare platform enables companies to better manage healthcare costs while delivering the industry’s highest member satisfaction
Dec. 21, 2017—San Francisco, Calif—Collective Health today announced it will enter 2018 with 30 enterprise clients, thereby doubling its client base, and 120,000 members across all 50 states and Puerto Rico. The company has expanded into new verticals including energy, real estate, retail, automotive, provider services, security, and manufacturing, complementing its existing presence in technology, financial services, aerospace, and consumer packaged goods.
“Innovative companies across the United States are realizing there is a better option when it comes to employee healthcare,” said Ali Diab, co-founder and chief executive officer of Collective Health. “By switching to Collective Health and combining their health plan administration, plan analytics, member decision support and engagement tools, and concierge-level member service into one system, companies are not only simplifying a tedious, antiquated process, they’re able to much better manage their healthcare cost trend and finally provide employees and their families a health benefits experience they love.”
2017 Savings Fueled by Collective Health and Product Momentum
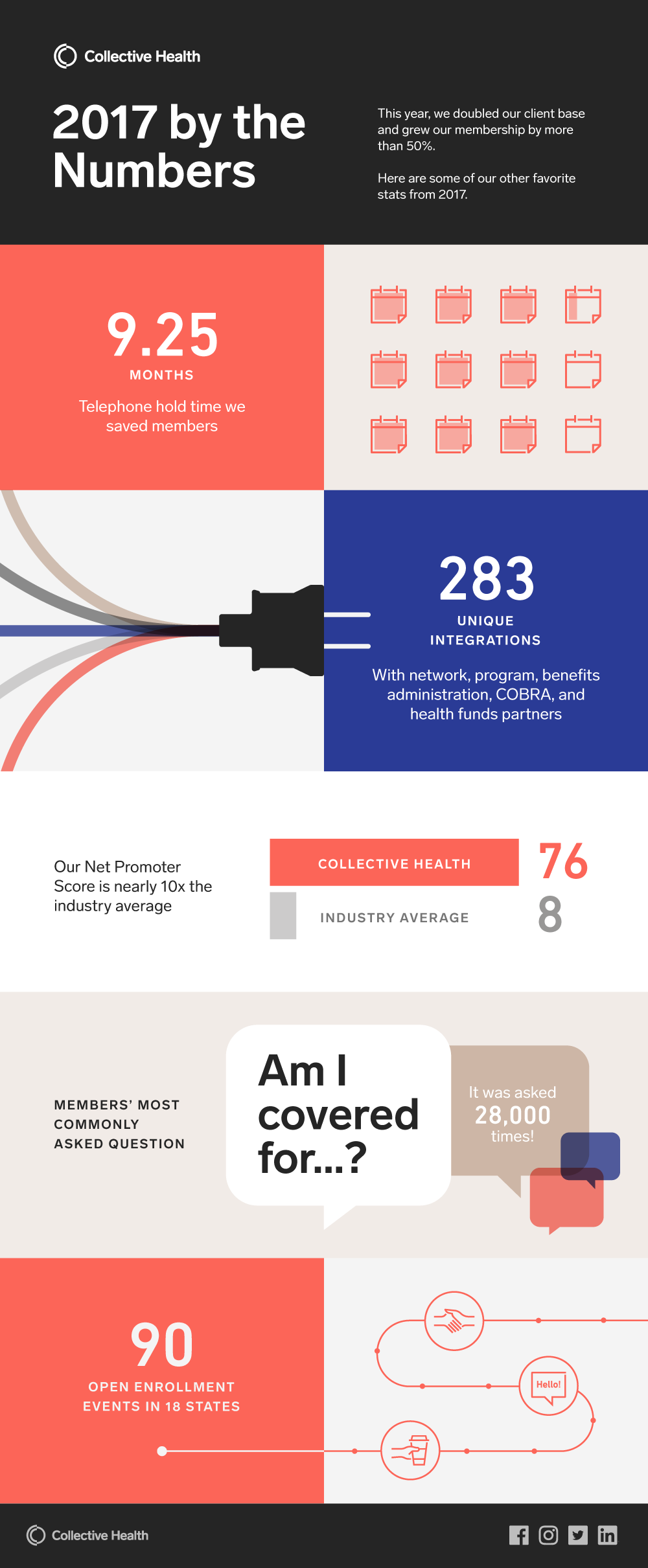
Collective Health’s all-in-one health benefits solution has helped clients manage costs while increasing access to care for their employees and families. In 2017, clients saw a negligible (0.1 percent) uptick in medical costs, in stark contrast to the 5 percent industry average increase. More importantly, members substituted less optimal care for more optimal services. For example, utilization of emergency room visits decreased by 5 percent, while urgent care increased by 4 percent. While specialists visits and advanced imaging went down by 8 and 12 percent, respectively, behavioral health services increased by 13 percent.
“In a time when we’ve come to expect medical costs to continue to rise without any measurable increase in health outcomes, we are thrilled we can help our clients defy expectations,” said Dr. Rajaie Batniji, co-founder and chief medical officer of Collective Health. “These early results reinforce our product’s simple premise—making it easy for people to engage with their health plan, and helping them get the right care at the right time, can quickly and meaningfully change the deleterious status quo.”
Members are increasingly using Collective Health’s digital tools to get the most from their health benefits—for example, members from 2016 used the web portal 36% more in 2017. This year, Collective Health released multiple upgrades to its digital tools and several new products that made engaging with healthcare more effortless, including:
- CareX, an intelligent system that improves member engagement by proactively connecting the right member to the right healthcare program at the right time. CareX is powered by Collective Health’s patent-pending analytics engine, Cortex. Since early 2017, Cortex has combined and analyzed more than 6 million innovative data points.
- An improved mobile application, with features including simplified out-of-network claims submission, health funds management, and cost and quality guidance. Available on iOS and Android, it’s intuitive, user-friendly design has fueled adoption that’s 4X the industry average.
- An integrated, full stack technology system to power Collective Health’s concierge support team, the Member Advocates. In addition to enabling Collective Health’s industry-leading member Net Promoter Score (NPS), this system was honored in Fast Company Innovation by Design awards.
The company also added 41 new network, program, benefits administration, COBRA and health funds partners; in 2017, Collective Health drove 283 unique partner integrations across its customers.
2017 Corporate Expansion
To facilitate its rapid growth without compromising its industry-leading customer and client satisfaction scores, Collective Health expanded its team. The company grew by 40 percent and built out its leadership bench with executives from SAP, Evolent Health, and QuinStreet, adding to its already impressive team from Google, NASA, Blue Shield, Aetna, and Willis Towers Watson.
Companies interested in learning more about Collective Health can visit https://collectivehealth.com/impact-for-your-company/
About Collective Health
Collective Health gives companies a smarter way to provide healthcare coverage through technology and design. Powered by an all-in-one solution that connects and administers the entire health benefits ecosystem—health plans, benefits programs, spending accounts, employee support—their technology delivers an effortless experience for everyone. Focused on serving the 170M+ Americans who receive healthcare coverage from their employers, Collective Health has been selected by leading U.S. companies. Founded in October 2013, Collective Health is backed by NEA, Founders Fund, Google Ventures, and other leading investors. The company is headquartered in San Francisco, Calif. For more information, visit https://www.collectivehealth.com.