Bring health benefits into the open.
See what’s driving cost. Build your benefits strategy on a unified foundation. Support your people with confidence.

An independent partner changes everything.
We’re the leading independent third party administrator (TPA) that brings together plan administration, cost management, and taking great care of your people — all in one place.
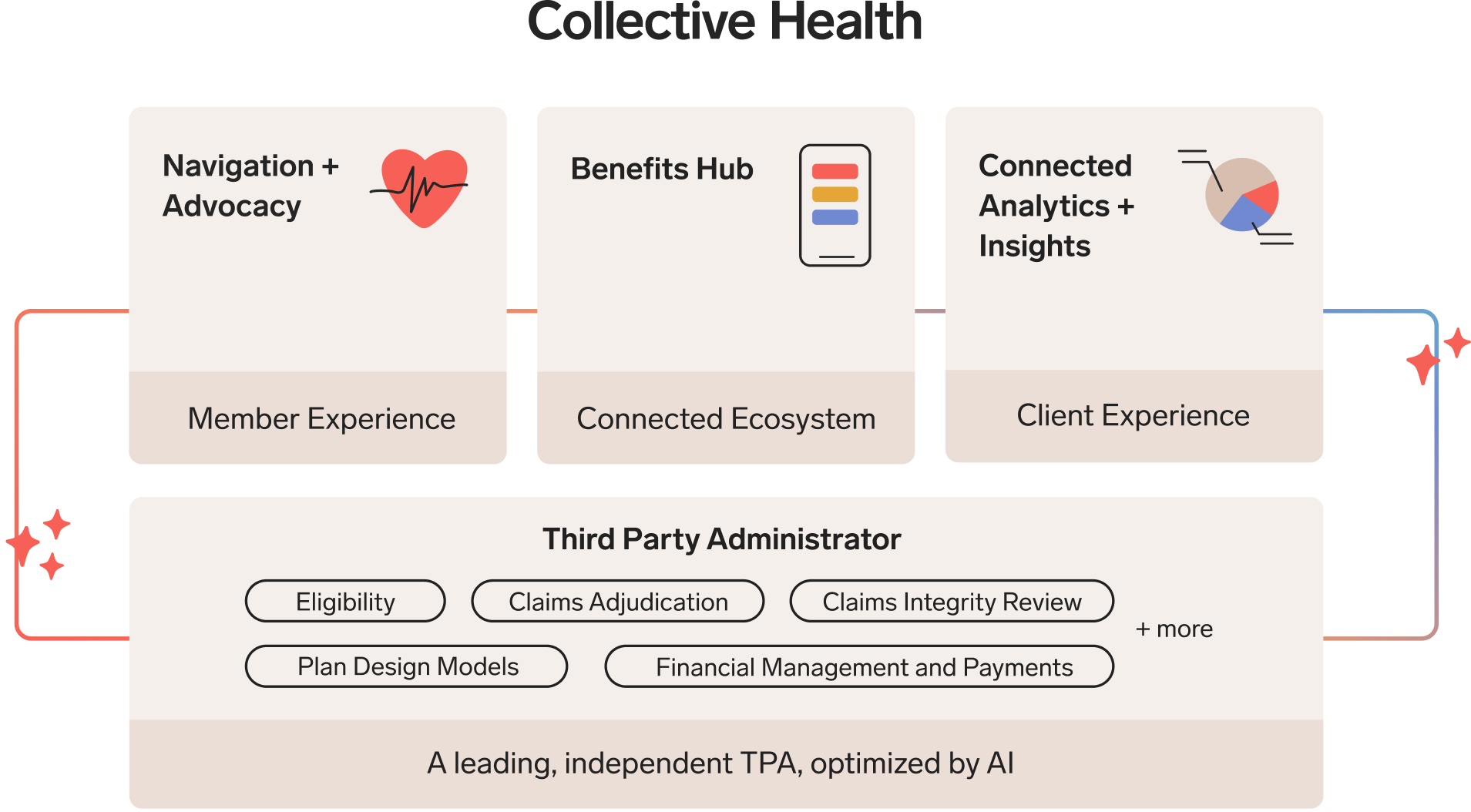
A higher standard for health benefits.
Clarity restores control. Transparency builds confidence. Aligned incentives drive results.
97%
of our revenue comes from PEPM fees. That’s it. No hidden fees.1
70
Net Promoter Score (vs health insurance industry average of 30)
$35
PEPM avg saved on a pre-paid basis with our claims integrity reviews. We catch mistakes the others don’t.2
$8,400
average savings per engaged member from Care Navigation.3
1 97% of revenue from PEPM fees: The remaining revenue is from one-time service fees, optional partner operational fees, and program administration fees.
2 Claims Integrity Review ($35 PEPM): Based on 2024 CH Book-of-Business client savings from CH Claims Integrity Review activities (e.g., duplicate claims, eligibility reviews)
3 Care Navigation ($8,400 per engaged member): Pre-post claims cost analysis (2024-2025)
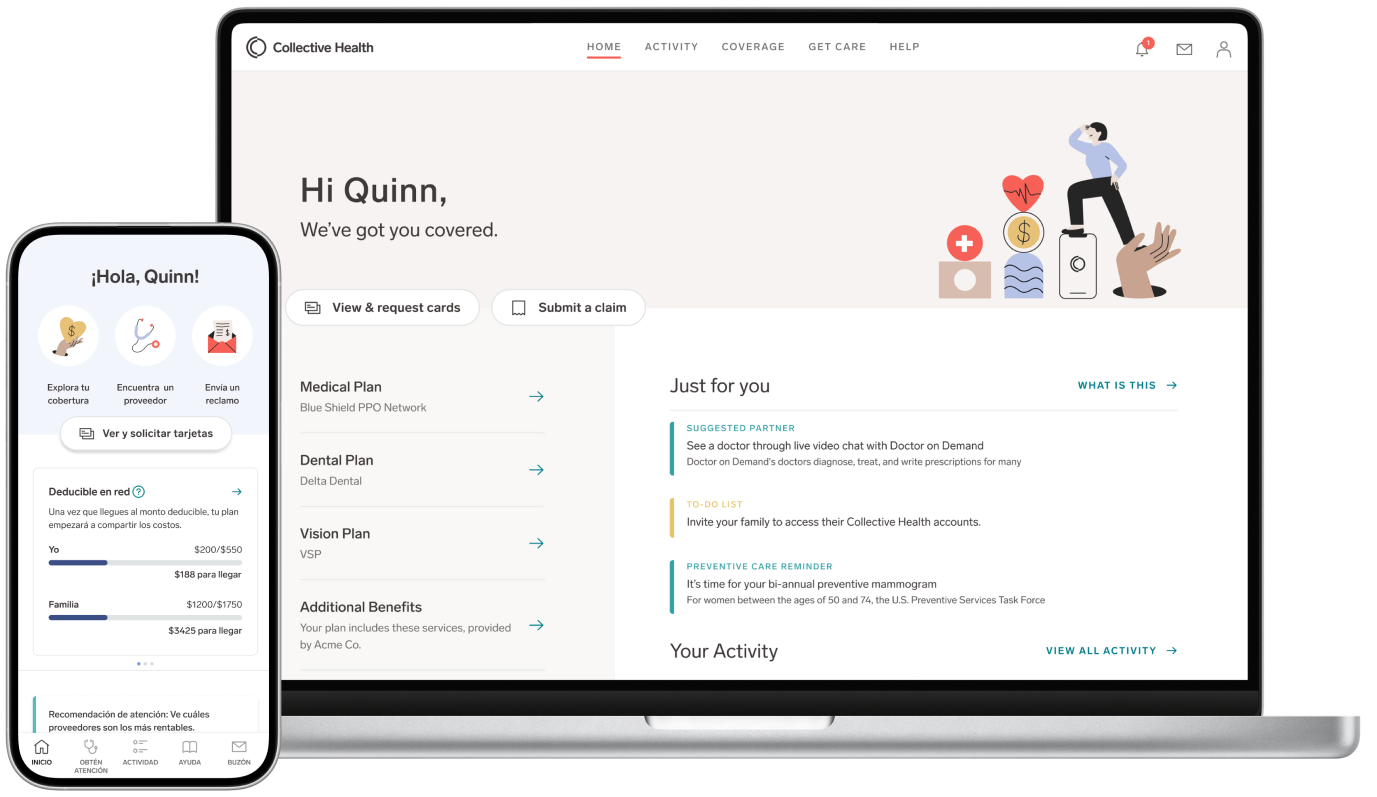
Stop managing your health benefits in the dark.
800,000+ members.
One connected solution.
No hidden fees.

Join other forward-thinking companies that trust Collective Health





