Platform-based approach to engaging members in the right care, and reducing administrative waste, makes a dent in American companies’ $1.2 trillion annual healthcare spend
Aug. 14, 2018—San Francisco—A new report from Collective Health shows the company lowered the cost of healthcare for clients from 2016 to 2017, while providing the industry’s leading member experience. With a -0.3% medical trend, Collective Health effectively decreased year-over-year costs, and saved returning clients an average of $500 per member family in 2017.
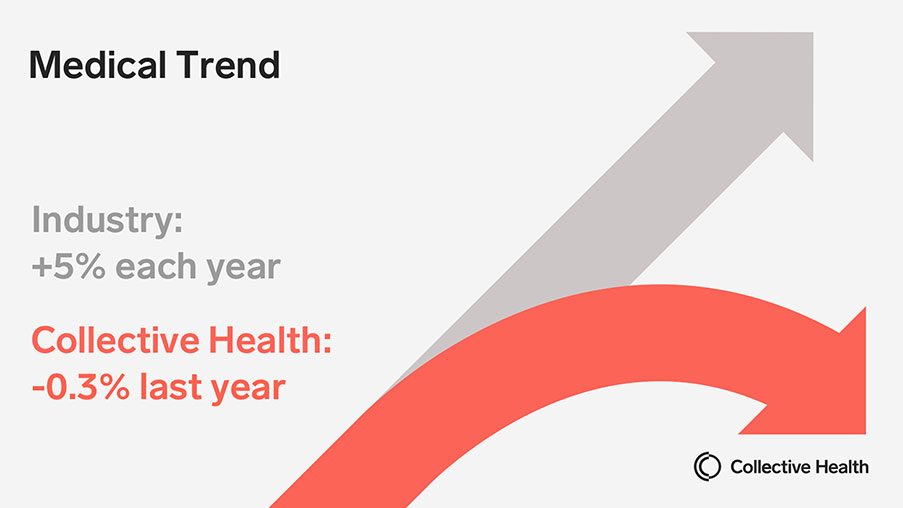
Collective Health’s approach addresses the increasing demand from the country’s largest private purchaser of health insurance, employers, that face dramatically increasing costs. According to a recent survey by the National Business Group on Health, national healthcare costs are expected to rise by 5% for the sixth consecutive year, with the expenditure per employee expected to hit nearly $15,000 in 2019.
Using its end-to-end Workforce Health Management System, Collective Health reversed the trend by helping its clients’ employees—Collective Health’s members—better understand their healthcare options, and find the right kinds of care. The report found the company also reduced billing errors, part of the administrative waste that is prevalent in healthcare.
“With our latest report, we can empirically say that we’re helping enterprises care for their people while effectively managing their healthcare spend,” said Dr. Rajaie Batniji, co-founder and chief health officer of Collective Health. “We’re doing so by addressing the technology problem that plagues health insurance. In the Employer-Driven Healthcare Economy, a software-driven approach—one that breaks down data silos to power intuitive products and unparalleled member support—can help lower costs by helping people get the right kind of care, not avoiding it.”
Collective Health released more details on the savings in its new “Controlling Employer Healthcare Costs” report. The report examines how focusing on three key elements can help employers lower the cost of healthcare while taking better care of their people.
Overall Medical Trend
Collective Health examined medical trend—the standard benchmark for measuring healthcare costs—for returning clients to quantify the change in healthcare costs per member from 2016 to 2017.
Trend for clients that have been with Collective Health since 1/1/2016 was an industry-leading -0.3%.
Member Engagement and Improved Decision Making
Diving deeper into medical trend, Collective Health found that a premium member experience—one that combines trust, simple language that helps people understand their options, intuitive product design, and the human touch—helps increase engagement and lower costs.

In 2017, returning members who engaged with Collective Health Member Advocates—the company’s dedicated in-house concierge support team—not only saw the biggest drop in medical trend (-0.8%), they also gave the experience a 70+ Net Promoter Score1.
Collective Health believes that a trusted relationship with members helps inform their care decisions, ultimately helping people optimize their choices. For example, Collective Health members reduced unnecessary specialist visits (-9.2%), and advanced imaging (-5%).
Intuitive product design can also help members find and optimize care. During the same time period, members increased utilization of telemedicine (+100%) and behavioral health care (+6%). Collective Health made it easier for members to access these services by:
- Tightening integrations with third-party telemedicine solutions, making it effortless for members to securely login to offerings directly from Collective Health’s web portal and mobile applications.
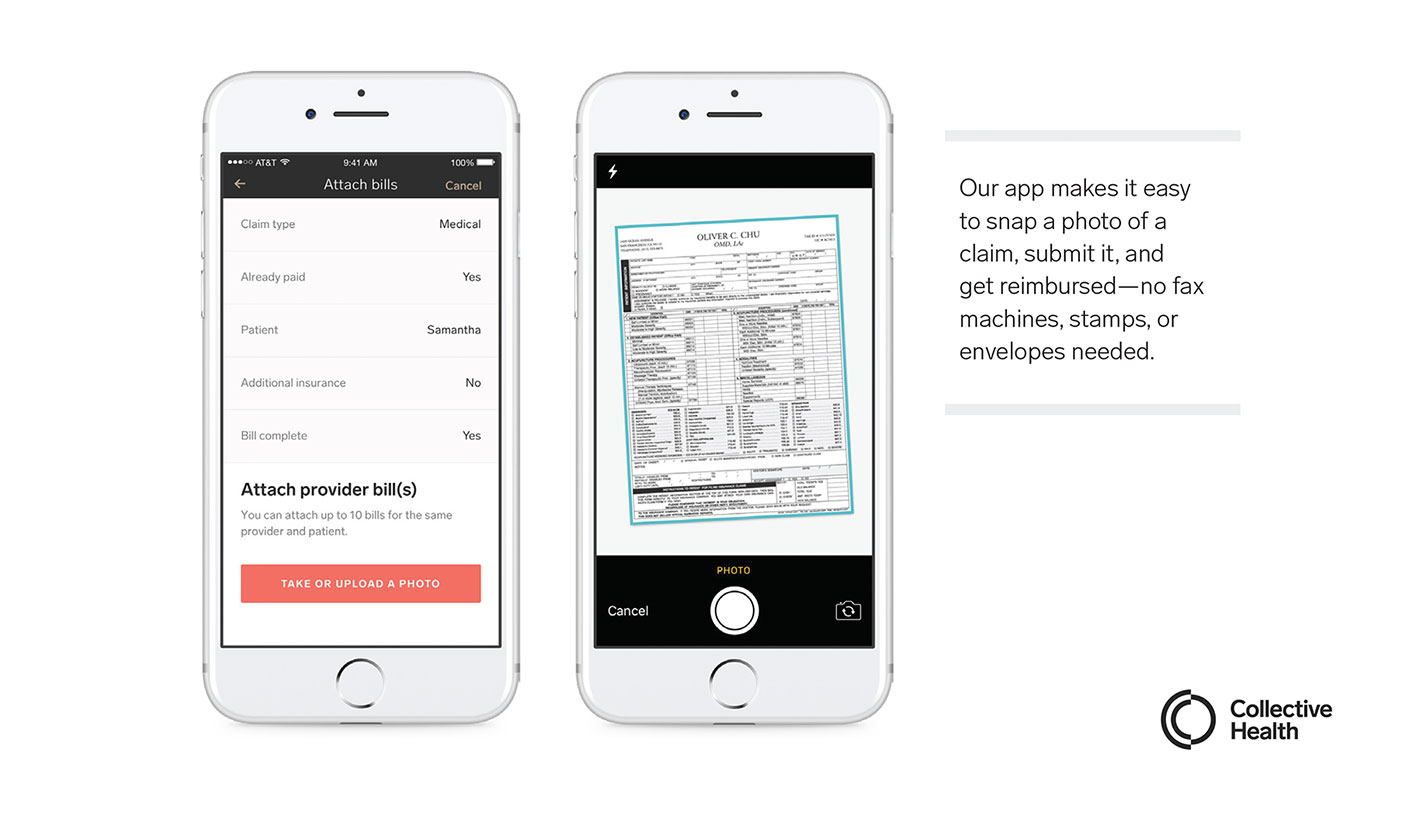
- Introducing mobile out-of-network claims submission, which alleviates the burden of getting reimbursed for out-of-network claims—an issue all too common in behavioral health care. This in-app feature allows members to snap a picture of a claim, submit it, and get reimbursed—no fax machines, stamps, or envelopes needed.
Administrative Waste
As the end-to-end solution that brings every part of a health plan onto a single platform and runs the financial side of healthcare for clients—from forecasting, to reviewing claims, and ensuring members pay the right out-of-pocket costs—Collective Health is uniquely positioned to identify and to fix common billing and administration errors.
In 2017, the company not only found errors in 57% of invoices from a subset of partners, Collective Health identified and fixed the errors before any erroneous payments were made.
The full report can be downloaded here.
About Collective Health
Collective Health is powering the Employer-Driven Healthcare Economy with the first Workforce Health Management System, giving employers a platform to simultaneously manage their healthcare investment and take better care of their people. With more than 120,000 members and 30 enterprise clients, Collective Health is reinventing the healthcare experience for self-funded employers and their employees across the U.S. Founded in October 2013 and headquartered in San Francisco, Collective Health is backed by NEA, Founders Fund, GV, Sun Life and other leading investors. For more information, visit https://www.collectivehealth.com.