Member experience sits at the center of everything we do here at Collective Health. It’s the foundation for how we empower people to live their healthiest lives. We know it’s impossible to empower people without providing them with a positive experience, and fast, reliable access to quality support. We are proud of our 70+ NPS (net promoter score) and >90% CSAT (customer satisfaction score), but we really measure ourselves by the feedback we hear directly from our members and our clients.
“This service has helped me so much with emotional support, education, access to medications, understanding bills, connecting me to resources, everything. I am so grateful.”
When designing our member experience, we prioritize connecting with our members where they’re most comfortable. Our support involves a combination of easy-to-use technology and the warm, human touch of our trusted Collective Care team—our team of Member Advocates, social workers, care coordinators, nurses, dietitians and pharmacists.
It’s all about connections
We view ourselves as the facilitators of critical connections for our members, which is why we provide them with advocates to help them navigate their journey. Does the member need a connection to a physician? A connection to understand their benefits? Do they need connections to various resources within the community? We not only make those connections for members, but constantly ask ourselves, how can we connect members to solutions in the most frictionless and warmest way possible? And sometimes that’s through one of our technology-enabled tools, and sometimes that’s through one of our Member Advocates.
What sets our experience apart
Our People
Our Collective Care team is focused on building out a group of prepared, capable and motivated Member Advocates and Care Navigators who create a best-in-class experience for our members. When recruiting, Collective Health looks for candidates who are naturally empathetic, creative problem-solvers.
We have developed a rigorous training program that combines customer service industry best practices with a clear, problem-solving approach. This way, we can ensure our team is equipped to help our members navigate even the most complex healthcare needs. Beyond the initial training program, we also provide recurring instruction to arm our staff with the latest information on any pertinent updates like new partners, tool changes, etc.
Before the go-live for a new client, our team is trained on each new client to understand their benefits, culture, and what is most important to them. We believe culture is important, so we work to understand specific nuances and priorities for the client, as well as preferences of the benefits team.
Our Technology
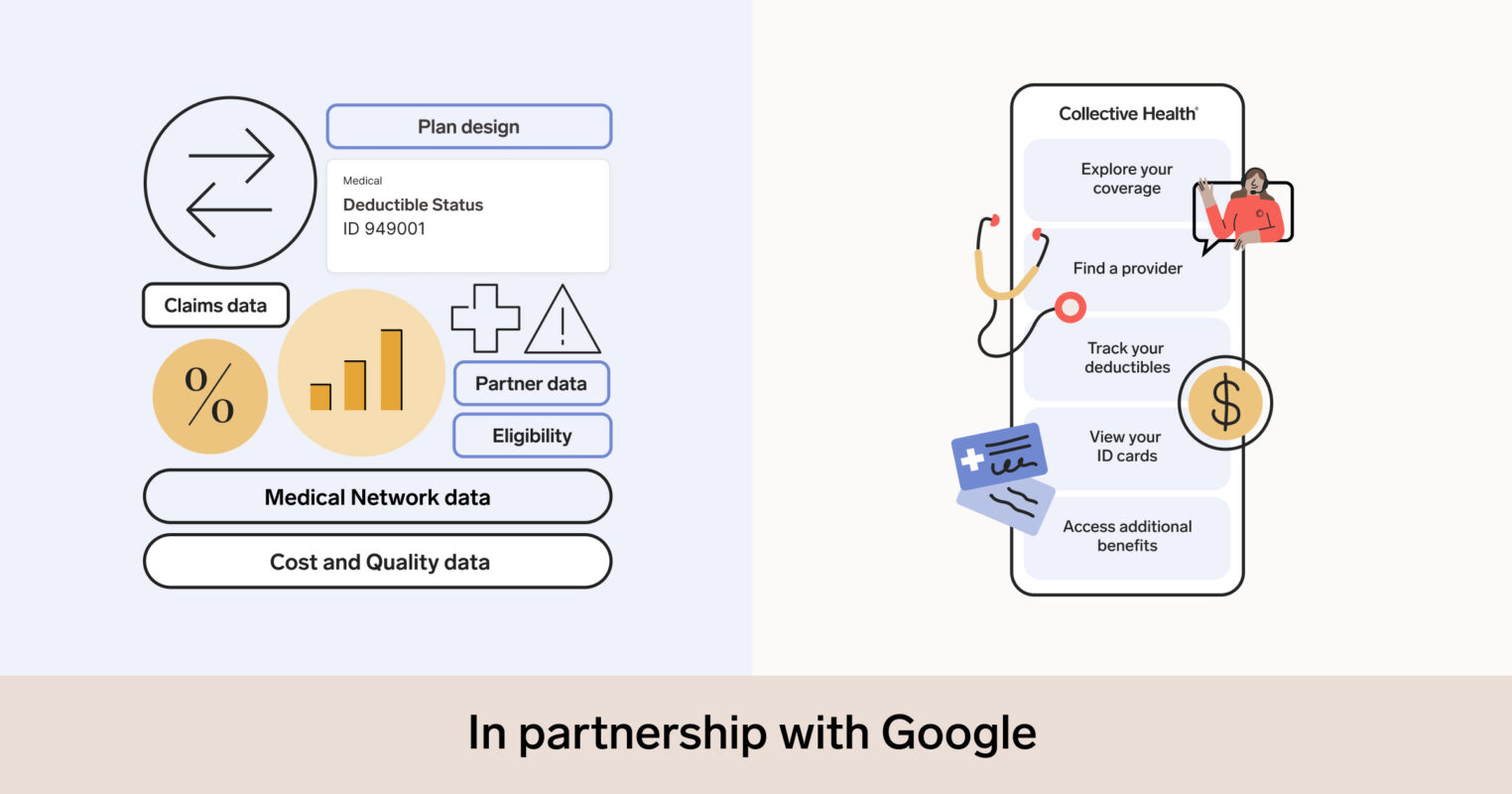
Whether members need to understand how their health plans work, review their claims, manage their spend, search for a provider, or submit a claim—our My Collective™ app brings everything together into one connected experience.
Before creating My Collective, our engineering teams developed countless prototypes and conducted thorough user research. Now, we continue to run ongoing studies with our members to understand how we can help empower our members with more effortless healthcare.
Just a few of the app’s features include:
- Intuitive benefit grouping: Plan benefits grouped by category, such as maternity and surgical care, which makes them easy for members to browse.
- Clear, direct language: Details of each benefit—such as the treatments included in a member’s specific plan—are written in clear and simple language, so members can understand exactly what is covered.
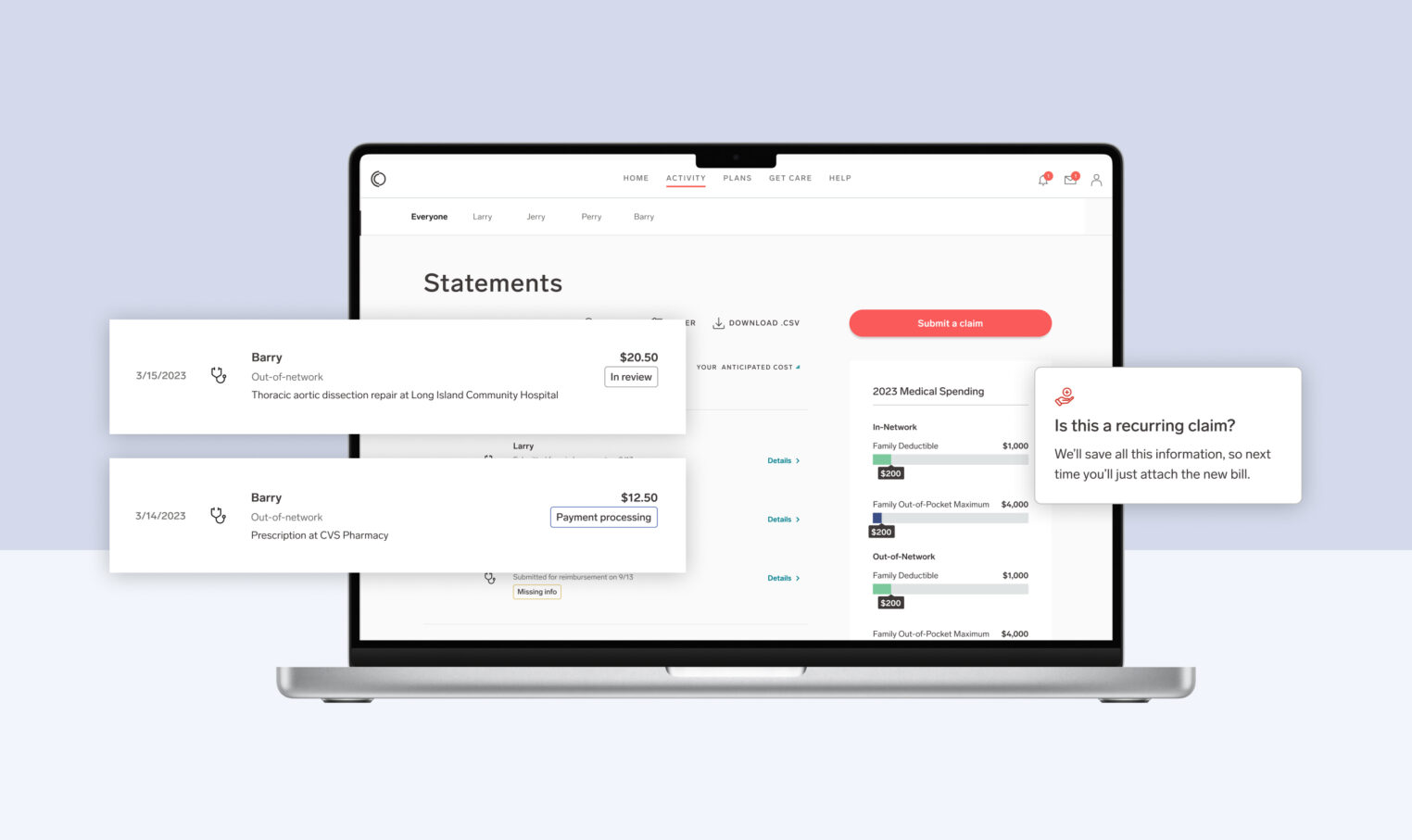
- Streamlined communications: Simplified EOBs (Explanation of Benefits Statements) show exactly what members are responsible for paying, and the information they need to follow up on.
- Frictionless claims submission: In-app ability to snap a photo of a claim, submit it, and get reimbursed—no fax machines, stamps, or envelopes needed.
A focus on quality
Member-led feedback: When evaluating the experience we provide to members, we measure the success of a member interaction differently than others. Our goal is to actually solve the member’s issue, not to get them off of the phone within a certain timeframe. We survey each interaction with our Member Advocates, and rely heavily on their feedback to determine our success. As a team, we openly celebrate positive feedback from our members, and closely analyze all our detractors that we can learn from.
Member-centric metrics: When we consider metrics like time spent, our approach is always member-centric (i.e., how do we not waste members’ time) versus Collective Health-centric (i.e., we were able to get through X number of calls in X minutes). Roughly 85% of the metrics we measure are related specifically to the quality of a member interaction.
1:1 Coaching: Our dedicated team of quality coaches helps to review our Member Advocate interactions so that we can ensure we’re consistently delivering the best experience possible. Our quality coaches provide 1:1 coaching for our Member Advocates, and also analyze any common hurdles or areas for improvement across the team.
Don’t take our word for it
Here’s a list of some direct feedback we have received from members:
“I’m always so impressed by the attention to detail, and nuance provided in answers to my questions.”
“[The Collective Health clinician] has been able to identify the best sources of care each time we have connected. [They] always followed up with me to make sure I was not putting it on the back burner and things were improving. I am really feeling [they] are a partner on my side.”