Industry
Social Media
# of Employees
9,000+
H.Q. Location
San Francisco, CA
Conversation with the
Head of Global Benefits at Pinterest
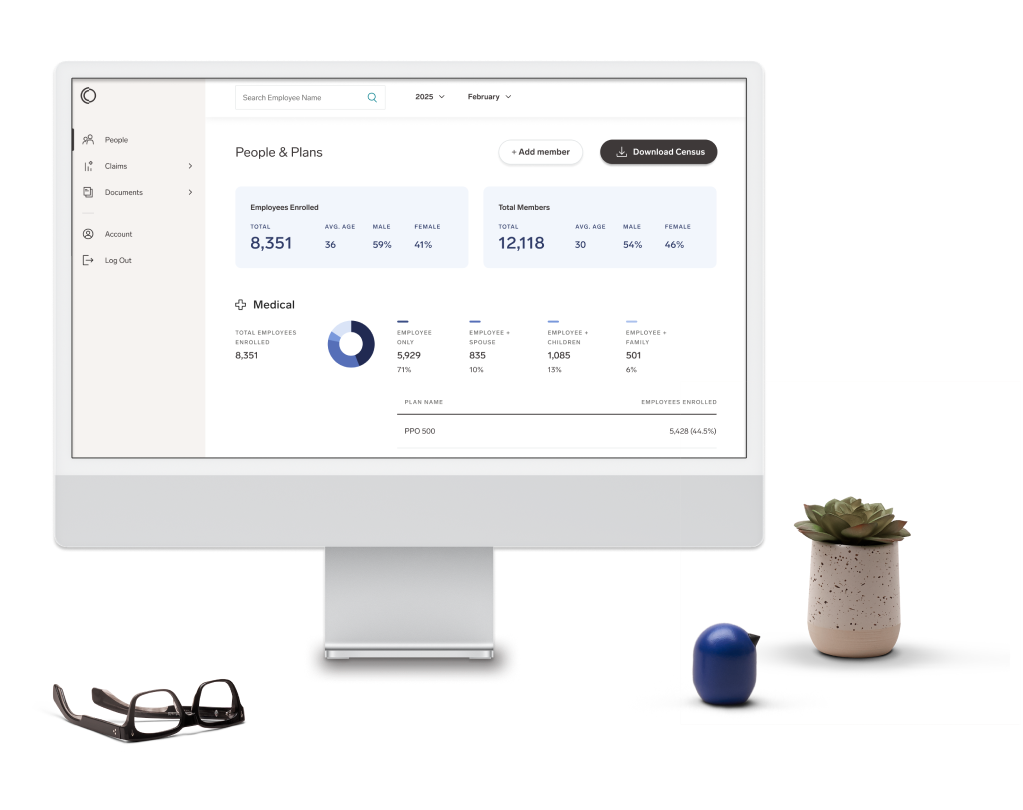
What’s it like to manage benefits at Pinterest?
Two things. First, benefits are a huge part of our people strategy. We compete for talent against a lot of brand name, larger tech companies, but we don’t have their level of budget to be able to do all the fancy things you hear about. Instead, we have to be incredibly thoughtful around what we offer, how we present our benefits while ensuring benefits are always relevant and helpful for our people.
Second, our employees are extremely engaged. They pay attention. They want to know more. They’re curious. That makes my job easier, but it also keeps me on my toes. They have high expectations, and if something isn’t quite right, we hear about it pretty quickly.
Ultimately, it all comes back to our company mission—to bring everyone the inspiration to create a life they love. If we want our employees to work on that, we want to make sure that our benefits strategy reinforces those ideals.

Before you made the move to Collective Health, what was keeping you up at night?
It was the constant struggles our employees had with our previous insurance company. Employees were upset that their claim was denied erroneously, or they didn’t understand a bill, or some related issue.
That was extremely frustrating for our benefits team because it points to a reality of our work. Nobody remembers how good health benefits are on paper, but everyone remembers what the experience is like. Despite all our effort and thoughtfulness, the traditional health insurance experience was letting us down.
What piqued your interest about Collective Health?
From the beginning, we got that Collective Health thought about the member experience differently.
It was designed around the member and what we, Pinterest, wanted to do for them. It was the type of healthcare experience our people wanted to have and the technology to support the experience.
From the beginning of implementation it was clear that Collective Health wasn’t just a vendor, they were going to be a true strategic partner.
What was the implementation process with Collective Health like?
Overall, the implementation went well. It was organized, really well thought out, and we were all on schedule. It’s definitely different than a traditional implementation because Collective Health is more deeply embedded in our day-to-day operations than a traditional health plan. But, from the beginning of implementation it was clear that Collective Health wasn’t just a vendor, they were going to be a true strategic partner.
How has Collective Health changed day-to-day administration for your team?
Like a lot of growing companies, we have a very lean benefits team, so we do everything from A to Z. We answer employee questions, we look into claims issues, and stay on top of the daily tasks. Switching to Collective Health has definitely taken work off of my team’s plate—that’s been great.
Now, we’re spending a lot less time directly dealing with member issues because we can confidently direct employees to Collective Health to get their questions answered. Last quarter alone, Collective Health answered more than 70% of all employee questions. The Member Advocates spend as much time as needed to help our employees choose and navigate their health plans. I’ve stopped getting emails from employees saying their question wasn’t answered. That was something we noticed immediately—even in the first 2-3 weeks of being with Collective Health we saw a huge drop in member issues.
Vendor billing and payments are another great example. It used to be a really time consuming piece of our job, but, now that Collective Health manages everything, that work just fades into the background.

How do you know if Collective Health is working?
First and foremost, we know it’s working because our employees are happily engaging with Collective Health directly. The data and surveys tell us that.
But it’s clearly working on the admin side, too. In benefits, I think we’re all used to being on the hamster wheel of trying to solve problems and errors. Just when you think you’ve reached the core of the problem, you get a brand new error report with 20 new records on it. You just never catch up. But, it’s been different with Collective Health.
WIth Collective, they take ownership and partner with us to find solutions to our problems. That feels so completely different. Now, when there are issues we typically only hear about them after Collective Health has already fixed them. It’s so refreshing to have someone proactively work on your behalf, especially when I had gotten so used to vendors saying that issues weren’t their problem to solve.
Collective Health makes it a lot more fun and satisfying to be on the benefits team of a great company like Pinterest.
How would you explain Collective Health to another benefits leader?
I could say a lot of different things depending on what that benefits leader is struggling with. But, fundamentally I’d say two things.
First, Collective Health is an amazing front end to your benefits strategy. They provide the technology and customer service that finally lives up to what you think your people deserve. I can’t tell you how many times I’ve heard our people say, “Have you tried the Collective Health app? It’s actually really cool.” I never thought our people would say that about their health insurance.
Second, they are an incredibly helpful back end. They do the basics like making sure people get their ID cards and claims are being adjudicated correctly. But they go way beyond that, too—they streamline eligibility, they take care of vendor payments, they help surface the data you need.
It’s pretty amazing to have a partner like that. Not only does it take a lot of the day-to-day work off your plate, it also gives you the confidence to make the strategic changes that you know will benefit your company and your people. Collective Health makes it a lot more fun and satisfying to be on the benefits team of a great company like Pinterest.
Want to see more about how Pinterest is driving a better benefits experience? Watch the video.
Interested in learning more about Collective Health?
Request a demo