User-centered design drives mobile adoption that’s 4X the industry average
The American healthcare system is full of paradoxes. We have the most expensive healthcare system in the world, but not the best health outcomes. Investment in mobile healthcare technology has been rapidly increasing and mobile accounts for 70% of our time online, yet people rarely use mobile to access and manage their health benefits.
When we started to design the Collective Health mobile experience, we sought to address this paradox by asking a simple question, “We use our phones to access almost everything, why shouldn’t we use them to access our health plans?”
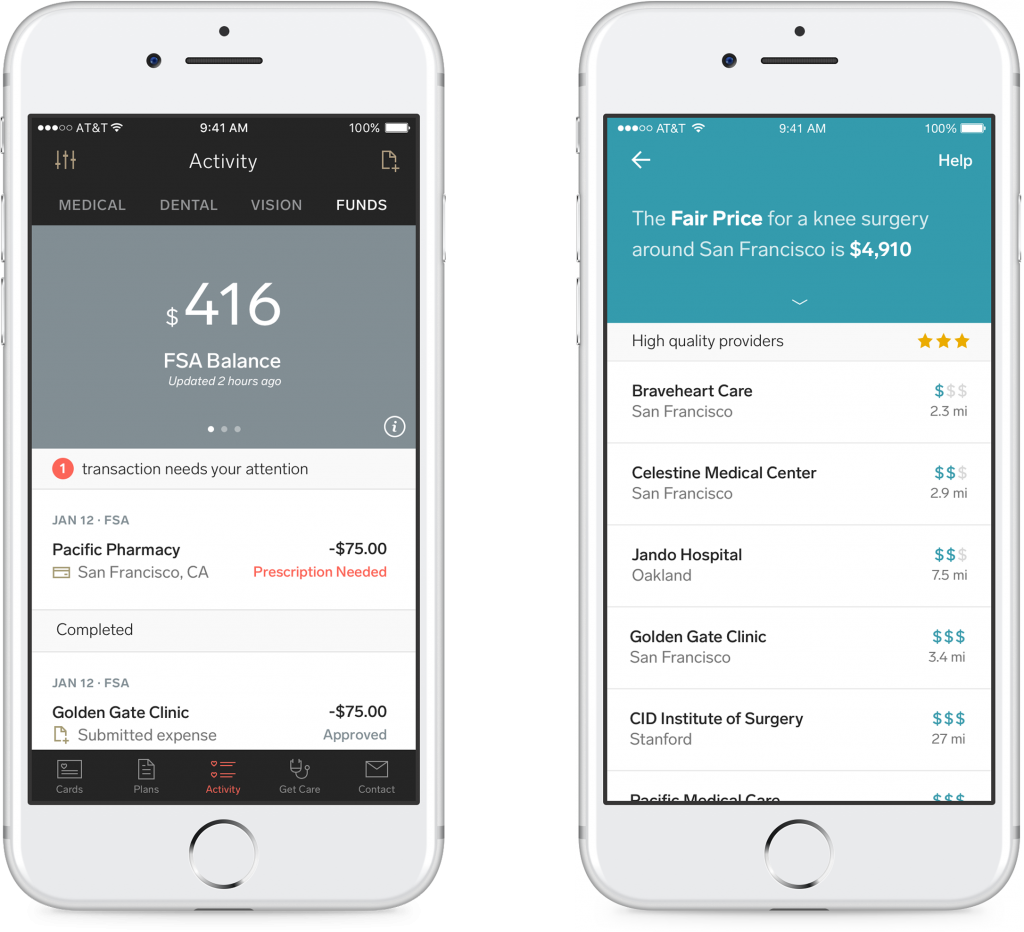
When we looked at existing health apps, we found that they tend to be confusing, difficult to log in to, and often times don’t work as expected—all problems we knew we could solve through effective design and engineering.
Our teams developed countless prototypes, conducted user research, and ran studies with our members to understand how an app could make accessing healthcare effortless. Through this process we identified four insights to shape our mobile experience:
- People have difficulty finding and understanding what’s covered in their plan. We grouped plan benefits by category, such as maternity and surgical care, making them easy to browse. The details of each benefit—such as the treatments included in a member’s specific plan—are written in clear and simple language, ensuring people can understand exactly what is covered.
- Doctors and pharmacists use the same medical card, but they have trouble finding the right information on the card. This results in member identification and insurance billing errors. Our mobile cards have different views for doctors and pharmacists that show each just the right pieces of information, making the point-of-care experience quick and painless.
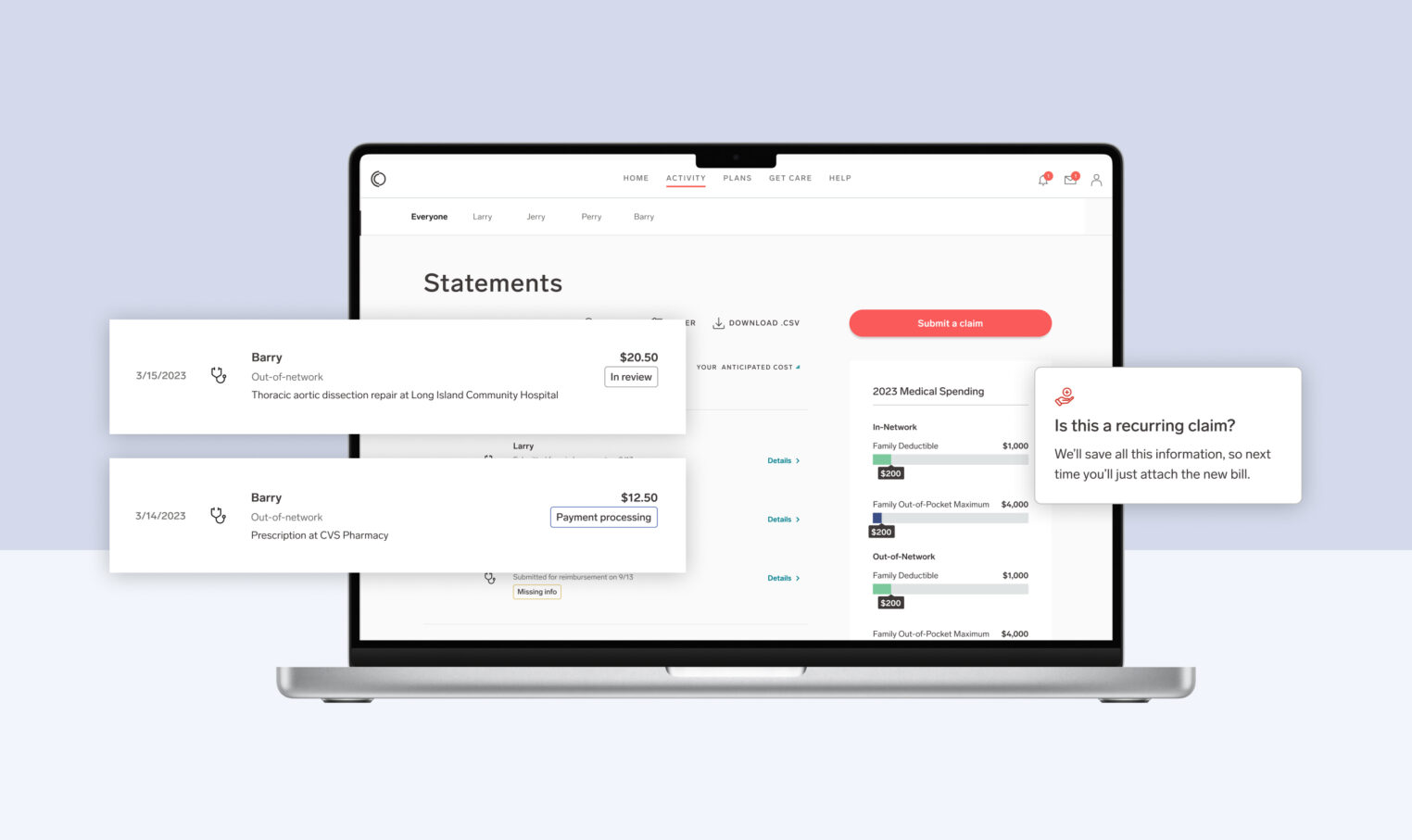
- After receiving care, people are confused about what they owe. We simplified our mobile Benefit Statements to show exactly what members are responsible for paying, surfacing the information that they need to follow up on. The best part? We designed it so members didn’t lose the ability to drill down into all of the details of their claims if they were looking for more information.
- People who go out-of-network are confused and burdened by reimbursement paperwork. Our app makes it easy to snap a photo of a claim, submit it, and get reimbursed—no fax machines, stamps, or envelopes needed. That means our members save time on paperwork and get reimbursed weeks sooner than if they had to deal with the antiquated process. They can also take these steps right at the point of care—that’s one less thing to remember after visiting the doctor.
In addition to addressing these insights, we focused on adding capabilities that make mobile truly shine. Remembering logins and passwords causes friction, so we built our iOS and Android apps to use Touch ID, Face ID, and fingerprint authentication. In our Get Care feature, we use your location to determine the closest provider to you, removing one more barrier to finding the right doctor.
In order to enable this experience we knew we had to avoid cross-platform interfaces and development shortcuts in favor of native code on iOS and Android—we are focused on using Swift, Java, and Kotlin. This allows us to use the latest capabilities offered by each platform, take advantage of great performance, and deliver a product that feels both familiar and comfortable to our users.
The impact of all this work? Adoption of our app is quadruple the industry average and it’s helping people get the most out of their health benefits—our mobile users log in 35 percent more often than web users. Most importantly, our members love our app and continue to find it to be the easiest way to access their health benefits.
“I love that I can access my health insurance card info from my phone. So convenient and easy to see my activity and what’s covered.”
– Collective Health member
We’re proud to deliver a truly mobile healthcare experience for the companies we support. It’s one where their employees (our members) don’t struggle to understand their benefits, can find the right care, and navigate their health benefits from wherever they are—whether it’s at work, home, the doctor’s office, or somewhere in between.
We believe we’ve set the standard for what a mobile healthcare experience should be, but we still have work to do. Our Design, Engineering and Product teams continue to improve and add new capabilities to our app, while we deliver a superior mobile experience to all our members.
You can find more details on the mobile application’s latest features here. If you’re interested in giving your employees the Collective Health experience, request a demo.