As a benefits leader, you likely field questions from your employees all day long regarding their health benefits. Where can I access my benefits information? What providers are in-network? How much will this procedure cost?
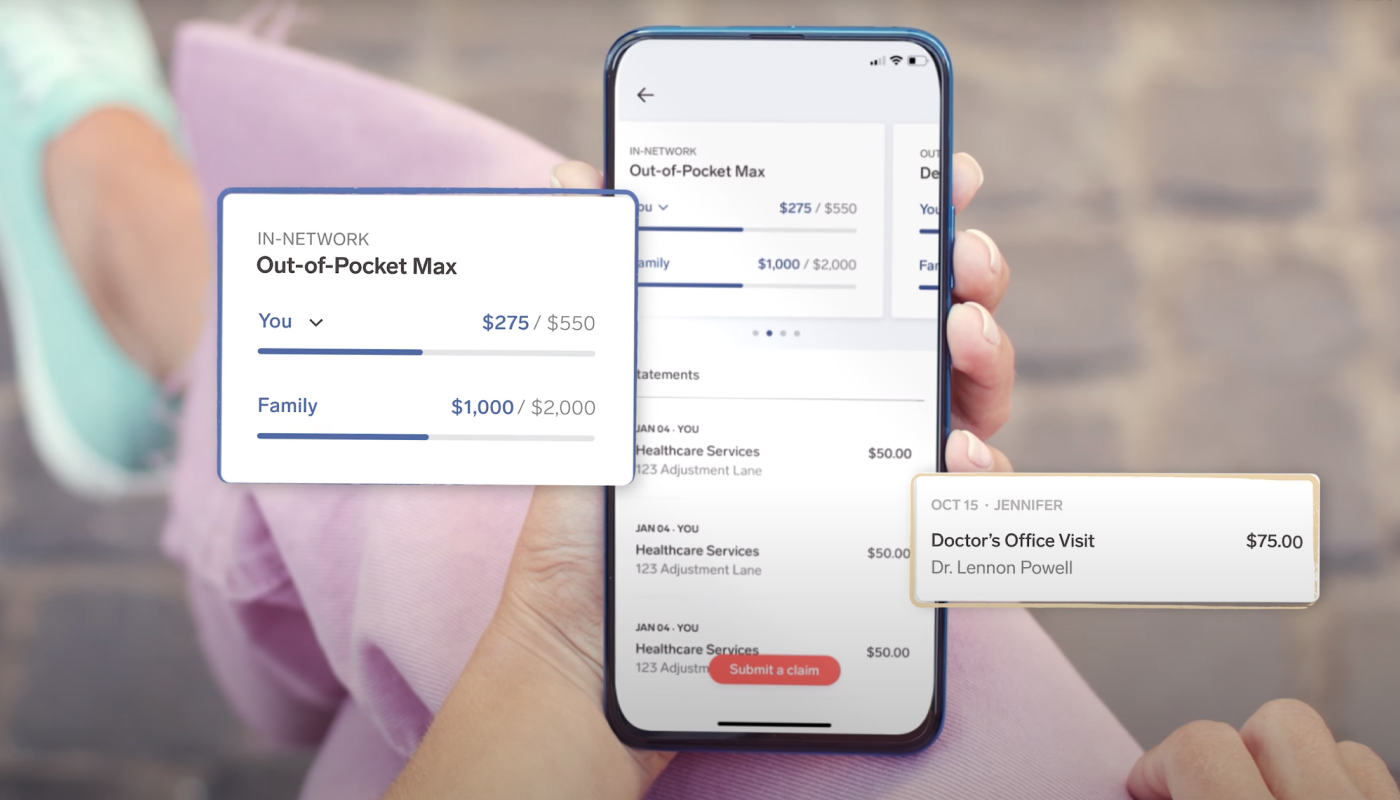
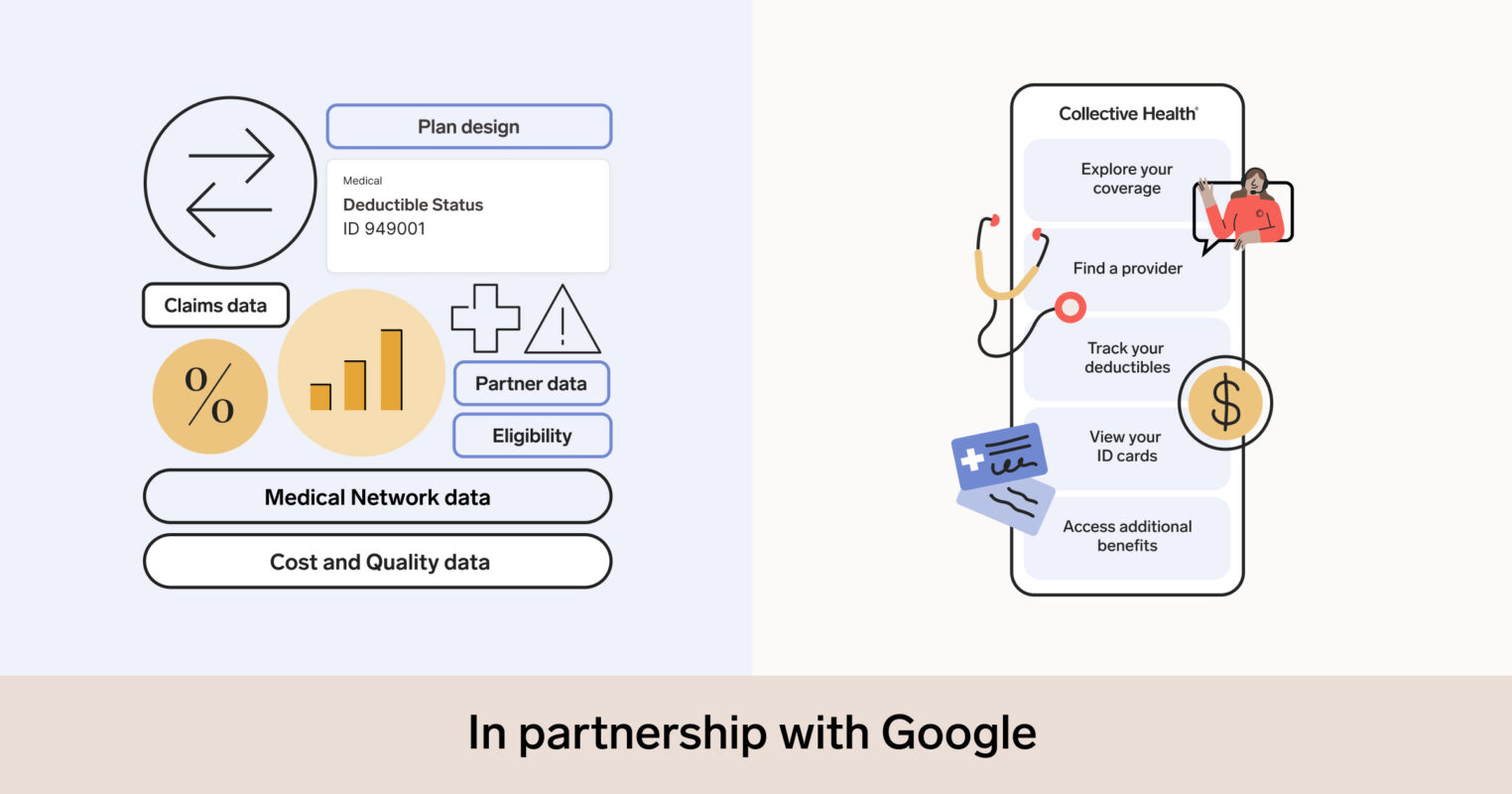
But if provided with the right resources, your employees can answer many of these questions themselves. At Collective Health, we built a digital experience that empowers our members to get answers on their own time in clear language that’s easy to understand. Whether accessing their benefit cards, searching for new providers, or getting a detailed breakdown of their plan’s coverage and prescription cost, we aim to make these answers simple and accessible. We’re always listening to member feedback on improving our product, which is why we’re excited to announce this roundup of recent updates to the My Collective™ experience.
Our Help Center just got even more helpful
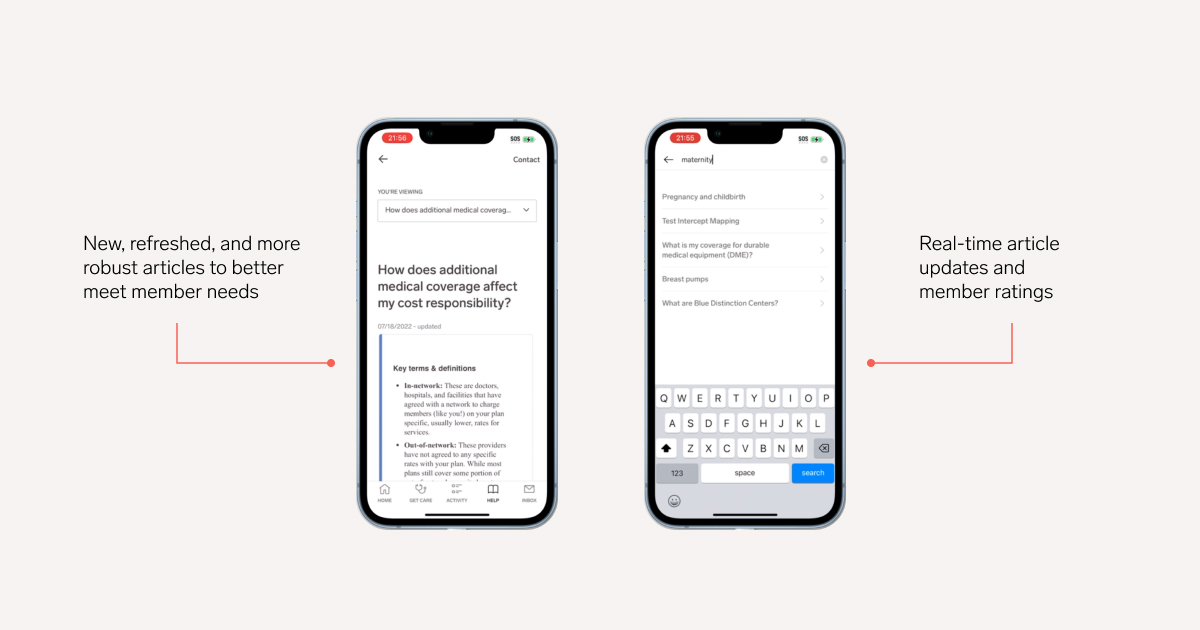
Our revamped Help Center makes it easier than ever for members to get answers to key questions. We’ve added 100+ new and refreshed articles about popular healthcare topics, including member benefits, claims, and more. We’ve also reorganized the structure of the Help Center into more intuitive categories for more straightforward navigation, combined related forms and documents for easier access, and dynamically ranked and promoted content so that members see trending topics on the homepage.
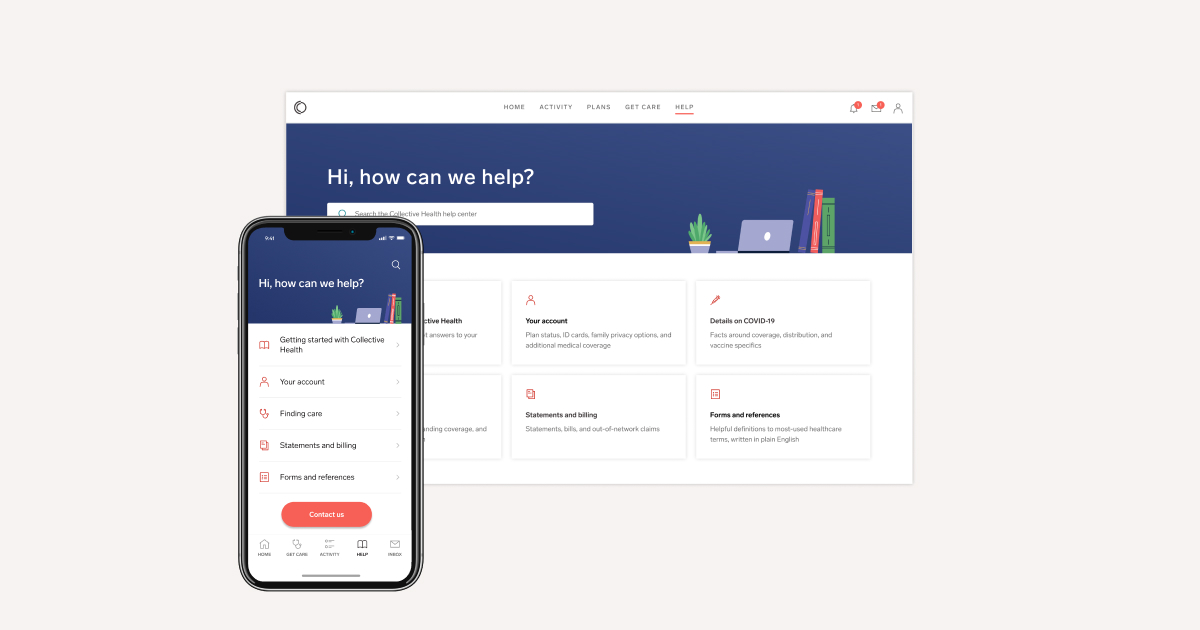
Why members will love it: Members will have more and better answers to their key questions at the touch of a button.
Why benefit leaders will love it: With members proactively getting their questions answered, this helps lessen the time you need to answer employee questions or escalate support issues to health benefits plans.
Easily search and compare costs for medical procedures
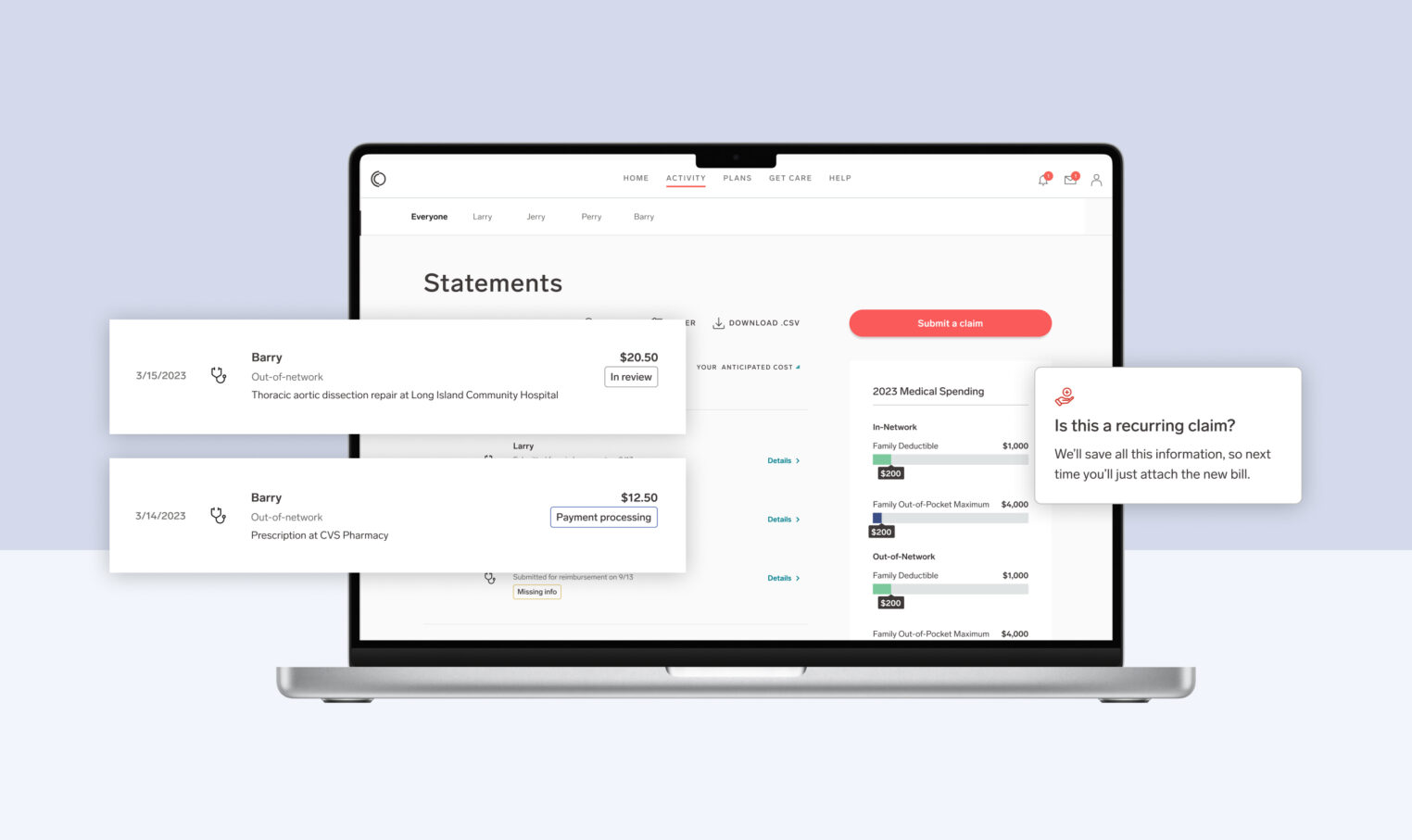
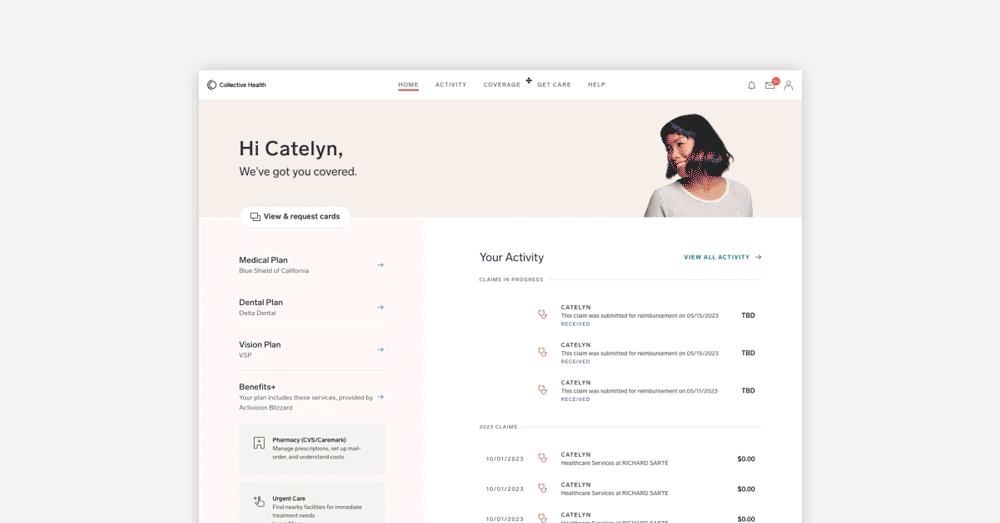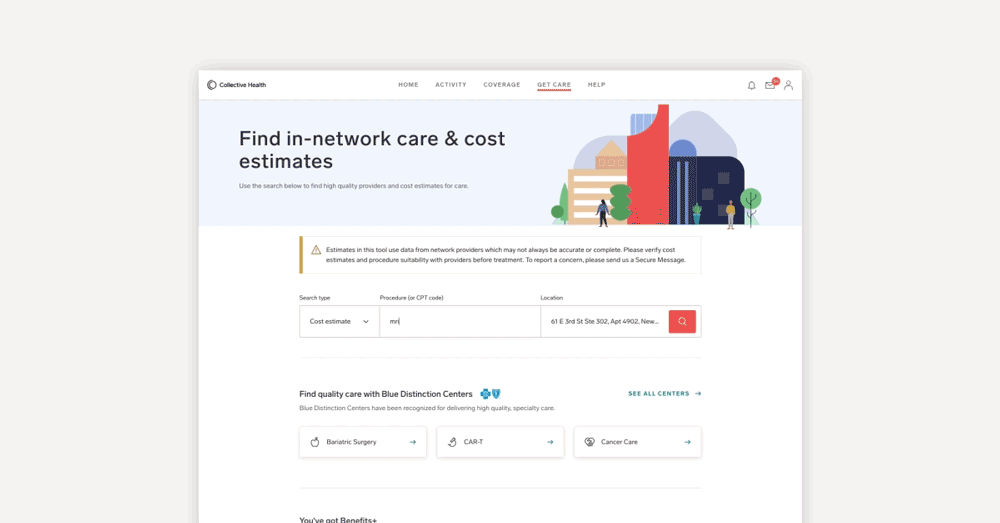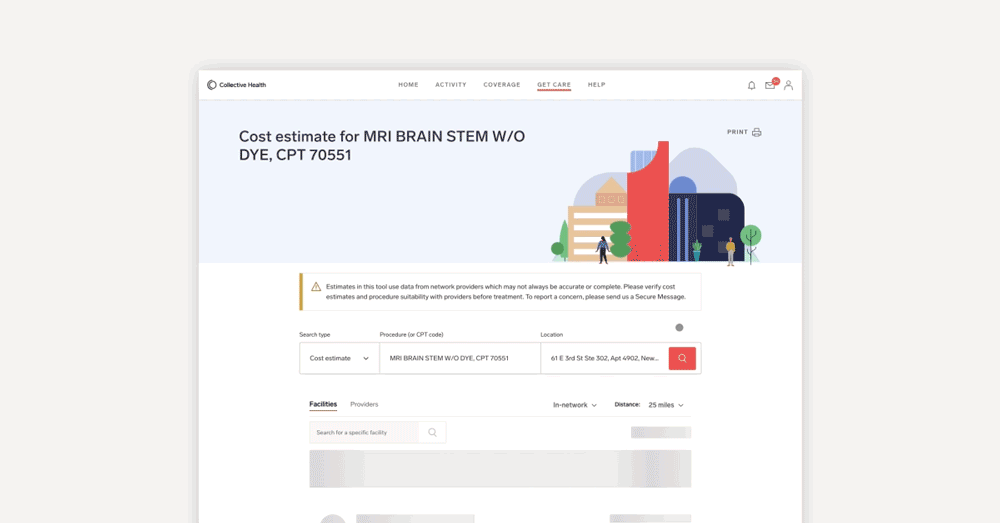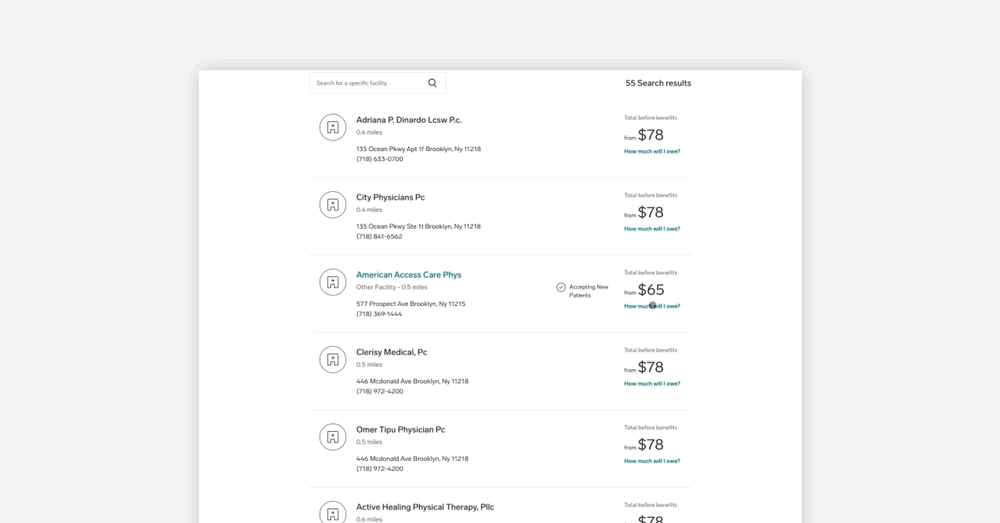
Searching for providers and estimated procedure costs just got simpler with the My Collective™ Cost Estimator tool release, built per the Transparency in Coverage Rule, which supports members in preparing for the costs of future medical services. Members can search for costs by medical procedure code or description, compare rates across in-network medical providers, and review estimated cost-sharing according to the employer and plan-specific benefit design.
How does it work? Within the Get Care page of My Collective™, a member can select a medical procedure (either by description, partial description, or procedure code) and select a location around which to center their search. The search results will show a list of medical facilities and providers within the specified area and the allowed amount for the service. The allowed amount shown is the negotiated price between the carrier network and the provider. Members can dig into each row and get a real-time estimate of the out-of-pocket cost.
What makes it different from other cost estimator tools? Cost estimation depends on data feeds from third-party network partners, which may contain inaccuracies that are also reflected in other cost estimator tools. Collective Health proactively seeks network partners’ resolution of errors in the data files they’ve provided us. As always, we advise members to consult providers to verify estimated costs before receiving care.
Why members will love it: Members can better understand their estimated out-of-pocket costs based on current medical plan coverage, including the total before benefits, the deductible amount applied to the visit/procedure, and then estimated out-of-pocket costs. This information will help them better prepare for the costs of future medical services and allow them to compare prices of procedures between medical providers.
Why benefit leaders will love it: This tool helps support your transparency in coverage obligations under the No Surprises Act and Transparency in Coverage rule.
Browse for providers by specialty and location
The Cost Estimator Tool works seamlessly with our Provider Search functionality, which enables members to browse for providers by specialty and location. Members can quickly see if a provider is accepting new patients and any designations of distinction that apply to facility results.
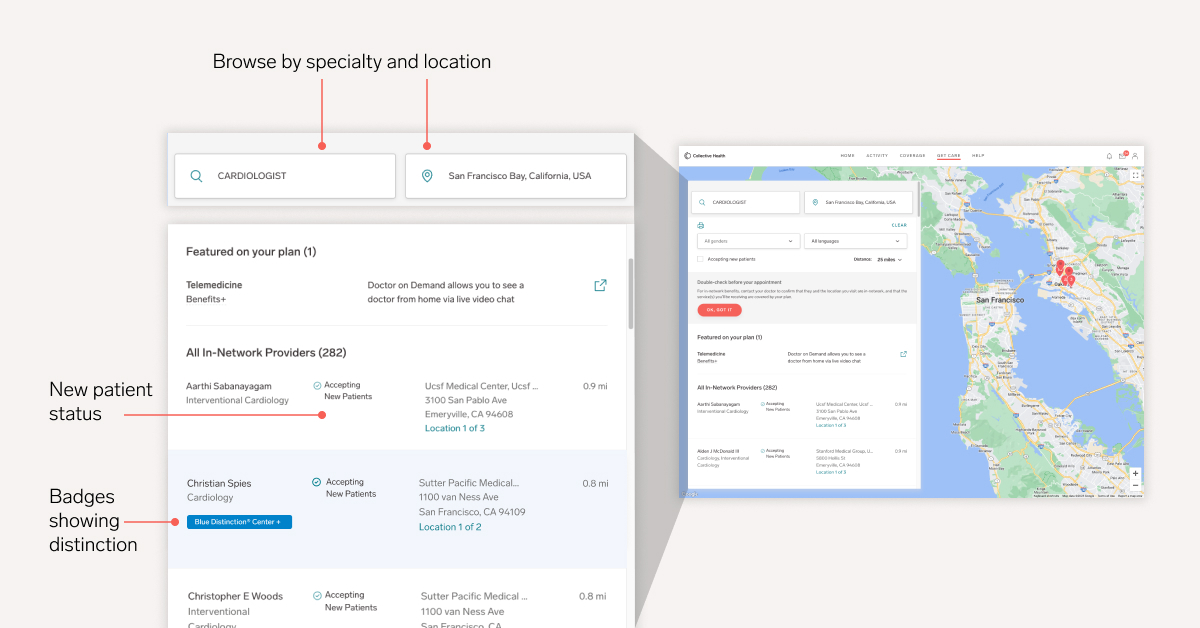
Why members will love it: Members don’t need to make a phone call for a list of in-network providers; the information is readily available online or in the app.
Why benefit leaders will love it: You’ll be able to point employees to the Get Care page or the My Collective™ app for any questions regarding providers in their area.